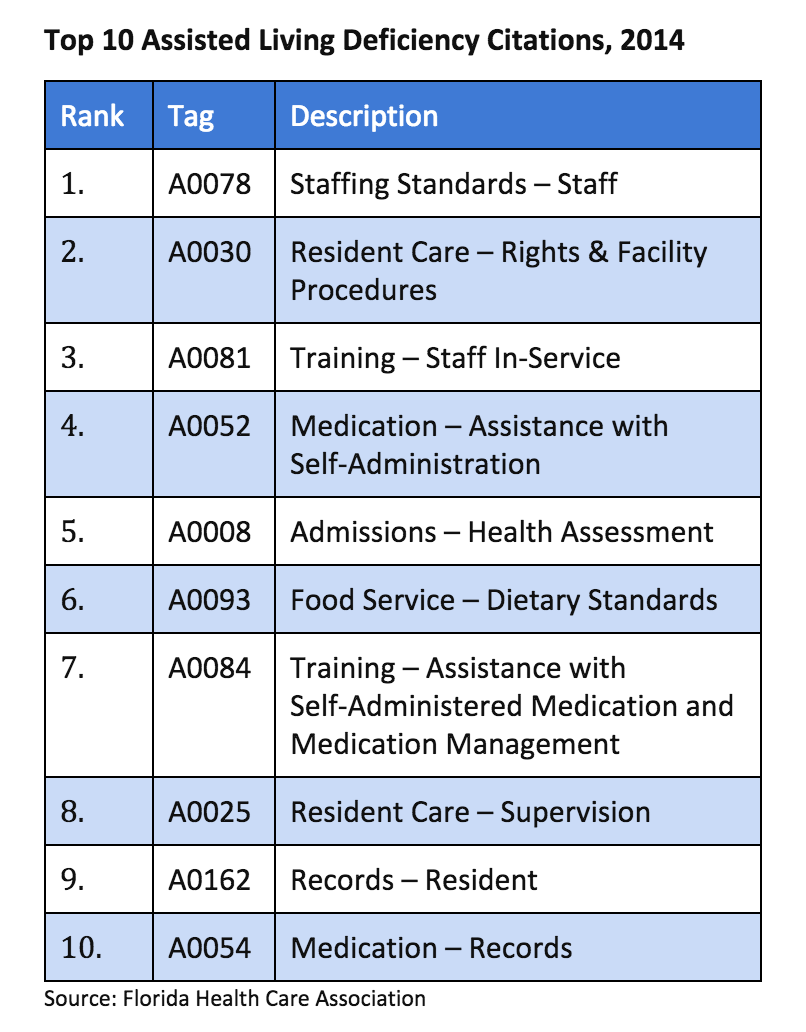
Staffing and resident care issues topped the list of reasons that assisted living communities in Florida were cited as deficient in 2014, according to Polly A. Weaver, assistant deputy secretary of health quality assurance for the Florida Agency for Health Care Administration and director of the state’s survey agency.
Weaver recently spoke at the LeadingAge Florida Annual Convention & Exposition. Her insights could be instructive to operators in other states as well, given the numbers of senior living providers and older adults in the Sunshine State. The retirement industry is Florida’s second-largest economic sector, serving 4.2 million adults aged 60 or more years, according to a fact sheet (PDF) from the Florida Department of Elder Affairs. Florida is the state with the greatest percentage of its population, 18.7%, aged 65 or more years, according to the Census Bureau.
The top 10 assisted living deficiency citations in 2014, according to Weaver:
-
Staffing standards. Employers must have documentation that their staff members do not have any signs or symptoms of communicable diseases and that they do not have tuberculosis. Also, employers cannot count RNs and LPNs as “healthcare providers.” Under Florida law in 2014, a healthcare provider is a physician, physician’s assistant or advanced registered nurse practitioner.
-
Resident rights and facility procedures. Survey concerns, Weaver said, relate to staff treatment of residents, ongoing physical plant issues, limiting access to the refrigerator by locking it, limiting resident access to the telephone, withholding food from residents as punishment, and the use of restraints other than half-bed rails.
-
Staff in-service training. Employers must document that staff members have undergone training on residents’ rights; reporting incidents; recognizing and reporting resident abuse, neglect and exploitation; residents’ behavioral needs; emergency procedures, including those related to resident elopement; and infection control, including safe food handling.
-
Assistance with self-administration of medication. Operators must follow the law regarding staff preparation of syringes for injections and the administration of other medications.
-
Health assessments. Providers must complete health assessments for all residents, all assessments must be current, and all forms must include information about the level of assistance a resident needs (particularly with medication) as well as the date and the healthcare provider’s signature.
-
Dietary standards. Facilities must follow the published menu and must maintain a food substitution log. Also, a dietitian must review the menu annually.
-
Training related to assisting with self-administration of medication and medication management. Employers must document that required training has been completed, and training must be provided by qualified individuals, such as registered nurses or pharmacists.
-
Resident care supervision. Operators must provide the level of care and services needed by residents in areas such as falls prevention, elopements and resident-on-resident assaults. Also, operators must follow up on significant changes to resident needs as appropriate.
-
Resident records. Facilities must ensure that residents sign their agreements/contracts. Also, facilities must record resident weights semi-annually for those receiving assistance with activities of daily living. And communities must have a record of residents’ healthcare surrogates, healthcare proxies and guardians, and they must be aware of the existence of power of attorney documents, where applicable.
-
Medication records. Medication observation records must accurately reflect whether a resident received the medication, there cannot be a discrepancy between the medication observation record and the medication label or order, and all medication observation records must be signed.
The Florida Agency for Health Care Administration has detailed the requirements (PDF) on its website.



