
A new report from the Centers for Disease Control and Prevention’s National Center for Health Statistics sheds light on the characteristics of the 30,200 assisted living and similar residential care communities that were providing long-term care services as of 2014.
“Findings on differences and similarities in supply, provision and use, and the characteristics of providers and users of long-term care services, can inform policy and planning to meet the needs of an aging population,” according to the report, titled “Long-Term Care Providers and Services Users in the United States: Data From the National Study of Long-Term Care Providers, 2013–2014” (PDF).
Highlights:
Location. The supply of residential care beds per 1,000 people aged 65 or more years was higher in the Midwest and West than it was in the Northeast and the South. Specifically, 42% of the communities were located in the West, 28.1% in the South, 21.8% in the Midwest and 8.2% in the Northeast. Metropolitan areas were the settings for 83.1% of communities.
Business model. 81.8% of communities were for-profit, 16.9% were nonprofit and 1.4% had government or other ownership. Chain affiliation applied to 56% of communities.
Size. One to 25 people were served daily in 67% of the communities, 28.3% served 26 to 100 daily and 4.7% served 101 or more people daily.
Staff. In 2014, about one-fifth of the all long-term care nursing and social work employees (more than 1.5 million nursing employee full-time equivalents — including registered nurses, licensed practical nurses or licensed vocational nurses, and aides — and about 35,200 social work employee FTEs) were employed by assisted living or residential care communities.
The most common employee type in assisted living/residential care was aide. Of the 332,400 FTEs in assisted living and similar residential care communities, 82% were aides, 10.7% were LPNs or LVNs, 6.5% were RNs and 0.8% were social workers.
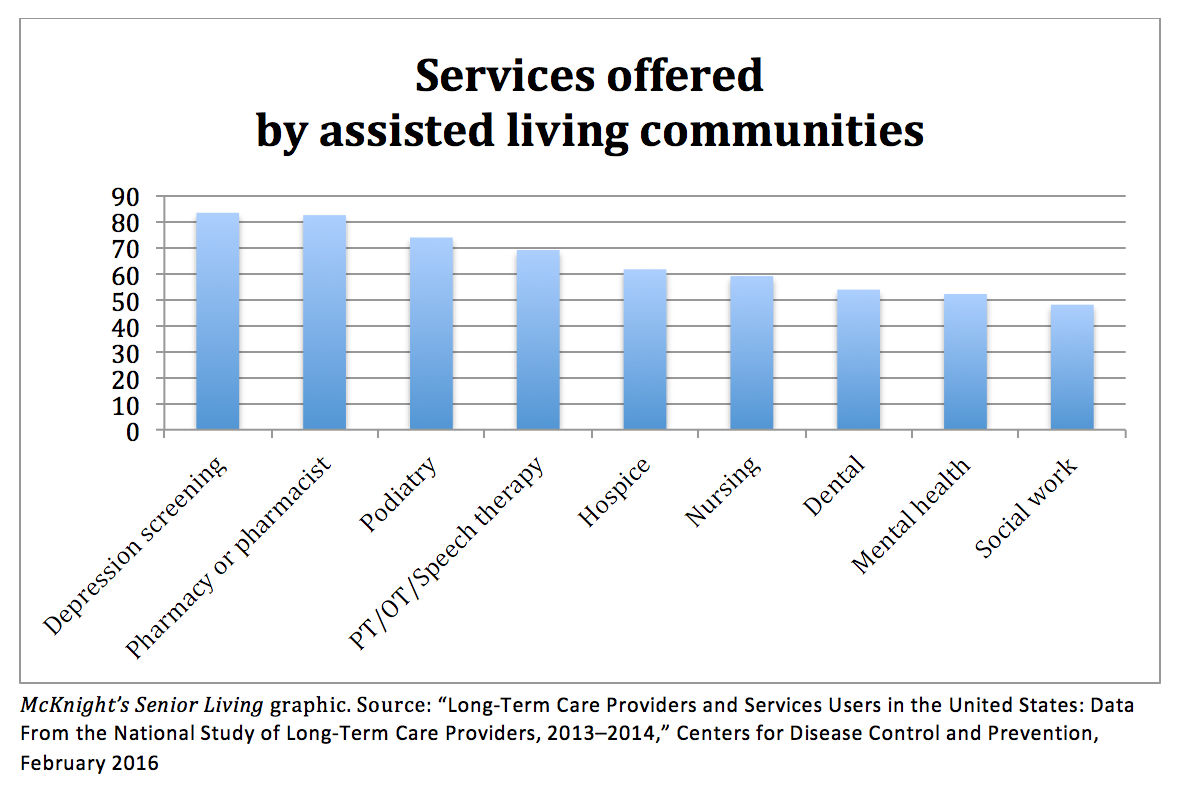 Services offered. Depression screening was the most commonly offered service, with 83.3% of communities offering it; 23.2% of residents had received a diagnosis of depression. Other services: pharmacy or pharmacist services (offered by 82.4%); podiatry services (73.8%); physical, occupational or speech therapy (69%); hospice (61.6%); nursing (59%), dental (53.8%), mental health or counseling (52.1%), and social work (48%).
Services offered. Depression screening was the most commonly offered service, with 83.3% of communities offering it; 23.2% of residents had received a diagnosis of depression. Other services: pharmacy or pharmacist services (offered by 82.4%); podiatry services (73.8%); physical, occupational or speech therapy (69%); hospice (61.6%); nursing (59%), dental (53.8%), mental health or counseling (52.1%), and social work (48%).
Alzheimer’s and dementia care. 77.8% of assisted living/residential care communities did not have dementia care units; 12.1% had a unit, wing or floor designated as a dementia care unit; and 10.1% served only adults who had dementia. Almost 40% (39.6%) of residents had received a diagnosis of Alzheimer’s disease or dementia.
The report details the current national picture of providers and users of services in five major sectors. In addition to assisted living, the sectors include adult day service centers, home health agencies, hospice and nursing homes. The NCHS plans to conduct the study every two years to monitor national and state trends.



