
The effects of a minimum wage increase on assisted living and continuing care retirement communities, and their workers, are multifaceted. On balance, however, such an increase could have a relatively small negative financial effect on operators but generally positive effects on their workers, according to results of a study released Tuesday by RTI International and the Center for Excellence in Assisted Living.
“Our study showed that the average financial impact of a $10 or $12 minimum wage would be relatively small for providers — 1 percent and 5 percent in total costs, respectively — but potentially important for the worker who makes only $7.25 an hour,” Joshua Wiener, Ph.D., a distinguished fellow at RTI and leader of the study, said in a statement.
 Costs for operators would be “substantially larger” related to a $15 minimum wage, however, Wiener said. Such a change would increase provider costs by a roughly 13%, he said.
Costs for operators would be “substantially larger” related to a $15 minimum wage, however, Wiener said. Such a change would increase provider costs by a roughly 13%, he said.
To arrive at their estimates, RTI researchers looked at four positions that are common in senior living communities: healthcare and other support aides, personal care aides, buildings and grounds staff, and food service workers. In fact, those types of jobs make up three-fourths of positions in senior living, researchers said.
They found that a minimum wage increased to $10 per hour would affect 27% of workers in those roles, an increase to $12 would affect 58% and an increase to $15 would affect 86%.
Tax issues vary by state, but as examples, the researchers estimated that increasing the federal minimum wage to $12 would require an annual wage and payroll tax increase of approximately $2,799 per worker in California and roughly $5,023 per worker in Texas.
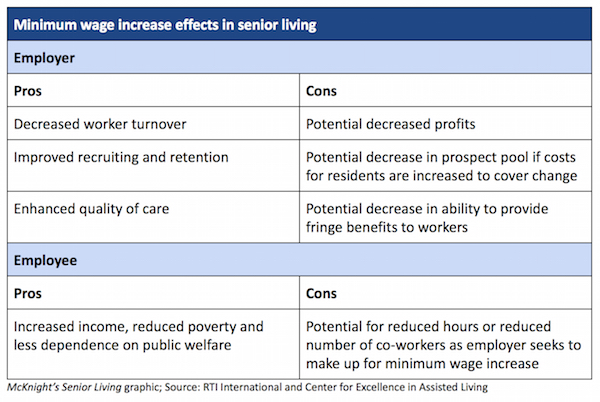
Although provider costs would increase along with the minimum wage, the report authors cited other research that minimum-wage increases could reduce poverty and the use of public assistance programs among workers, improve staff recruitment and retention for employers, and increase the quality of care.
Noting the challenges facing operators, Lindsay Schwartz, Ph.D., board chair of CEAL, said, “There is a constant need to attract and retain staff who can provide quality care, and there’s also the challenge of keeping costs affordable for individuals and families who rely on these communities.”
Schwartz also is senior director of workforce and quality improvement at the American Health Care Association/National Center for Assisted Living. Among the other 10 members of CEAL are the American Seniors Housing Association, Argentum and LeadingAge.



